Choosing the weight loss operation best suited for you typically means choosing between the sleeve gastrectomy operation and the gastric bypass operation. These two operations are by far the most popular weight loss operations performed in the United States.
Before we discuss the strengths and weaknesses of the gastric sleeve and the gastric bypass, let’s first discuss how popular each of the operations are.
The gastric bypass operation has been in use for more than 40 years, and has been the most popular operation for weight loss during most of that time. Over the past 10 years however, the popularity of the gastric bypass has been exceeded first by the LAP-BAND for a brief time in 2009 and 2010, and more recently by the gastric sleeve operation from 2013 to the present.
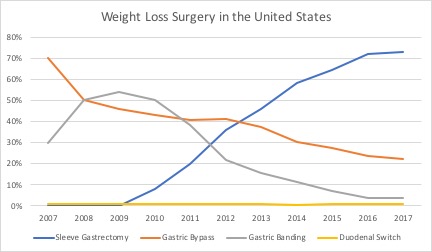
As you can see from the graph below, the gastric sleeve operation has grown tremendously in popularity over the past 10 years, and shows no sign of slowing down.
For first-time weight loss operations, about 73% are gastric sleeve operations, and 22% are gastric bypass operations. The remaining 5% are split between duodenal switch operations and LAP-BAND operations.
To summarize this data in a different way, the gastric sleeve operation is felt to be the ideal choice for about ¾ of weight loss surgery patients, and the gastric bypass operation is felt to be the ideal choice for about ¼ of weight loss surgery patients. The LAP-BAND and duodenal switch operations are felt to be the ideal choice for only a small fraction of patients.
Before we get to the details of how to choose the best operation for you, let’s briefly review the sleeve gastrectomy operation and the gastric bypass operation.
Sleeve Gastrectomy
The sleeve gastrectomy operation involves laparoscopically reducing the size of the stomach from approximately 30-40 ounces in volume to approximately 4 ounces in volume. Over time, this small stomach volume will expand to approximately 6-8 ounces in volume.
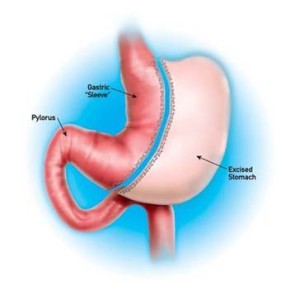
The gastric sleeve operation has been established to be safe and effective for weight loss.* Read more about gastric sleeve surgery.
Gastric Bypass
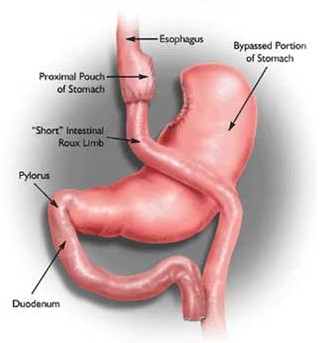
The gastric bypass operation involves laparoscopically creating a very small stomach pouch (approximately 1 ounce volume), and connecting the small stomach pouch to the intestine. The reconfiguration of GI tract anatomy results in food bypassing most of the stomach, and the first 2 feet of intestine.
The gastric bypass operation has been established to be safe and effective for weight loss.* Read more about gastric bypass surgery.
How to Choose – Gastric Bypass or Gastric Sleeve?
Both operations have been established to be safe and effective for weight loss, but let’s compare the safety and effectiveness of both operations in detail.
Safety – Surgical Complications
Both operations are considered to be safe, but the gastric sleeve operation is safer.* Because the gastric sleeve operation preserves more normal GI tract anatomy, it is a less invasive operation, and therefore lower risk.
A large published study (134,142 patients) entitled “Is Laparoscopic Sleeve Gastrectomy Safer than Laparoscopic Gastric Bypass? A Comparison of 30-Day Complications Using the MBSAQIP Data Registry” found that serious complications within 30 days of surgery occurred half as frequently after sleeve gastrectomy surgery than after gastric bypass surgery.*
Winner: gastric sleeve
Effectiveness – Weight Loss
Both operations are highly effective for weight loss. Both are thought to work by changing the biology that regulates body weight. This change in biology results in a change in body weight set-point to a lower weight.
Published studies show that, on average, gastric bypass results in more weight loss (by a small margin) than gastric sleeve. Average weight loss after gastric bypass is approximately 70% of excess weight, and average weight loss after gastric sleeve is approximately 60% of excess weight.*
Of note, different surgeons and programs achieve different average weight loss results – some surgeons and programs achieve better weight loss outcomes than others. Our weight loss outcomes, for example, average approximately 75% of excess weight for both gastric bypass surgery and gastric sleeve surgery.*
Winner: gastric bypass (just by a little)
Effectiveness – Diabetes Remission
Weight loss results in improvement in type 2 diabetes. The anatomy change involved with the gastric bypass operation results in further improvement beyond what occurs with weight loss alone.
In general, published studies report that remission of diabetes (normal blood sugar, no medications) occurs in 50-80% of patients after weight loss surgery.* Remission is generally reported to occur in a higher percentage of gastric bypass patients than gastric sleeve patients.
To learn more read the following key studies on weight loss surgery and diabetes:
Bariatric Surgery versus Intensive Medical Therapy for Diabetes – 5 Year Outcomes
This is an excellent randomized controlled study (the best kind of study) with long-term follow-up.
Comparison of Gastric Bypass with Sleeve Gastrectomy for Morbid Obesity or Diabetes: a Meta-Analysis of Randomized Controlled Trials
This is a review study of the published randomized controlled trials comparing gastric sleeve and gastric bypass for diabetes.
Predictors of Remission of Diabetes in Severely Obese Individuals Undergoing Bariatric Surgery: Do BMI or Procedure Choice Matter? A Meta-Analysis
This is a review study of the published studies on diabetes remission after gastric bypass and gastric sleeve.
Winner: gastric bypass, but gastric sleeve is not far behind
Effectiveness – GERD Resolution
Gastric bypass surgery generally resolves gerd (gastro-esophageal reflux disease). Gastric sleeve surgery usually improves gerd, sometimes makes gerd worse, and occasionally makes gerd severe. Generally, the more severe gerd is before surgery, the higher chance there is for gerd to be severe after surgery.
In my experience, severe gerd occurs infrequently in patients without a significant preoperative issue with gerd or hiatal hernia.* In patients with preexisting severe/chronic gerd and/or large/chronic hiatal hernia, the chance for severe gerd after gastric sleeve surgery can be 20% or even higher.
Winner: gastric bypass
Impact on Eating
The gastric sleeve operation preserves a more normal experience of eating than the gastric bypass operation.* This is because GI tract anatomy is preserved in a more normal state with the gastric sleeve operation.
The gastric bypass operation, on the other hand, more substantially changes the normal GI tract anatomy, and this more substantially changes the normal experience of eating. Patients generally adapt well to the eating changes after gastric bypass surgery, but in my experience, patients appreciate the more typical experience of eating that occurs with the gastric sleeve operation.
Winner: gastric sleeve
Summary
The most common operations for weight loss are sleeve gastrectomy and gastric bypass. Between the two, the sleeve gastrectomy has become significantly more popular.
The sleeve gastrectomy operation is less invasive, lower risk, and preserves a more normal experience of eating.* These are all compelling strengths of the gastric sleeve operation.
The gastric bypass operation results, on average, in more weight loss and is better for diabetes and gerd.* Because of these strengths, the gastric bypass operation is often favored in patients who are more overweight (BMI>50), or have diabetes (particularly more severe diabetes), or have severe/chronic gerd or a chronic/large hiatal hernia.
In these specific groups of patients (BMI>50, diabetes, severe gerd) it is felt that the added benefits of the gastric bypass operation outweigh the increased risk of the gastric bypass operation.
Learn more about Dr. Oliak and his Los Angeles and Orange County weight loss surgery program.
* Patient outcomes vary after weight loss surgery. Individual patients can do better or worse than the average.
More Weight Loss Surgery Resources

David Oliak, M.D.
Dr. Oliak is a board-certified, fellowship-trained surgeon who specializes in minimally invasive (laparoscopic and robotic) weight loss surgery. He has been in practice in Orange County, California, since 2002, has completed more than 3000 weight loss operations, and has a track record of excellent patient outcomes.*
Dr. David Oliak is the founder of the Oliak Center for Weight Loss. He started the Oliak Center because he wanted to provide weight loss surgery done right. His commitment has always been to provide the kind of care that he himself would want to receive. Dr. Oliak is affiliated with only the best bariatric hospitals and surgery centers in Los Angeles County and Orange County.
* Individual patient results vary. Past performance is not a guarantee of future results.
Which weight loss surgeon is right for you?
Download this guide of questions to ask your weight loss surgeon to help make the best decision for you.